Provider Credentialing Services
Get Credentialed Faster. Start Billing Sooner.
Credentialing is the foundation of your revenue cycle. Without proper enrollment and payer approval, your claims can’t be processed.
At Mbclaims, we manage the entire credentialing process — from application submission to payer approval — ensuring accuracy and faster turnaround times.
Our Credentialing Services Include
✔ Provider Enrollment (Medicare, Medicaid, Commercial Payers)
✔ CAQH Registration & Maintenance
✔ Re-Credentialing & Revalidation
✔ NPI Registration & Updates
✔ Contract Negotiations Assistance
✔ Group & Individual Enrollment
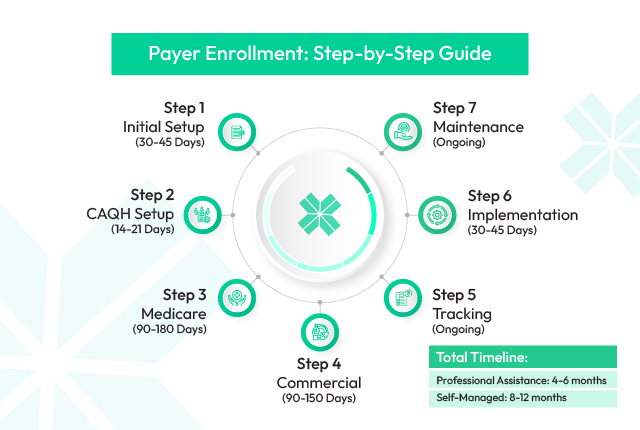
Why It Matters
Delays in credentialing mean delays in revenue. Our structured process minimizes errors and accelerates approvals.
With Mbclaims, you gain:
-
Faster onboarding
-
Reduced application rejections
-
Ongoing compliance management
👉 Let’s Get You Credentialed Quickly & Correctly.
